
Information governance in healthcare is relatively new, with focused efforts beginning in 1997. What started as an effort for healthcare providers to comply with regulatory and information security requirements has grown into comprehensive programs that also aim to deliver high quality data insights to enhance healthcare outcomes.
Today, health care organizations are fine tuning their data management policies and procedures to better manage data quality, privacy, and security. The evolving regulatory requirements and massive data growth with volumes tripling every three years forces an urgently needed roadmap to keep the organization’s data secure, accessible, sharable and compliant.
With medical mistakes ranking as a leading cause of death in the United States, there are many efforts underway across all continuums to improve patient safety and outcomes. From a health data standpoint, there is a significant shift toward data governance as a top priority in healthcare organizations according to a recent survey.
The role of carrying out governance program policies is the job of data stewards who oversee the organization’s data governance policies.
Bottom line: To fully realize the benefits of health data requires a concerted effort with a commitment to data governance’s guidance and data stewardship’s actions.
What is health data stewardship and why is it important?
Quite simply, data stewardship involves the day-to-day management and oversight of healthcare’s data assets to ensure their quality, consistency, and accuracy. The role of data stewards is becoming more prominent as the demands for healthcare data continue to expand.
Data stewardship includes overseeing every aspect of the data lifecycle and follows the organization’s established data governance policies.
Benefits of a solid stewardship program can help the organization realize advantages that include:
- Improved data quality
- Enhanced data security and privacy
- Better decision making
- Regulatory compliance
- Improved data accessibility
- Efficient data integration
- Cost savings
The Role of Health Data Governance and Stewardship in Healthcare
Both data governance and data stewardship hold key responsibilities in successful data management. Both disciplines are related and increasingly complex due to the skyrocketing growth of health data volumes and the increased interoperability requirements from the 21st Century Cures Act.
Data governance is the umbrella that covers the overall data management policies for an organization. AHIMA’s definition of Data Governance: The overall administration, through clearly defined procedures and plans, which assures the availability, integrity, security, and usability of the structured and unstructured data available to an organization.
Information Governance (IG) involves: “Minimizing information risks and costs while maximizing information value,” according to Information Governance expert Robert Smallwood, MBA, CIP, IGP.
The data governance market is on a rapid growth trajectory with a valuation of $3.27 billion in 2024 to $8.03 billion by 2029. This represents a CAGR of 19.72 percent.
This growth has fueled 90 percent of large companies including healthcare organizations to employ dedicated team members such as a Chief Data Officer to oversee governance, analytics and security which helps ensure regulatory compliance, operational efficiencies and supports data-driven decision making.
The main difference between data governance and data stewardship is that governance programs help ensure overall data integrity and security through policies, standards, and procedures. Data stewardship entails the implementation of the rules. Boiling it down, governance is the framework, and stewardship is the operational actions that follow the framework.
Health data stewardship is crucial in managing a data warehouse (i.e., all the data within an organization). This includes six key areas:
- Data Quality and Integrity. Includes conducting regular audits and quality checks to ensure high data standards are met.
- Security and Privacy. Champions ethical data practices for responsible data use, with a focus on privacy and security in all activities.
- Data Integration. Ensures data from various systems is consistent and compatible. This is increasingly important with AI and analytics initiatives.
- Data Accessibility/Interoperability. Ensures data is stored in an environment and in a source that can be accessed and shared. Facilitates seamless data exchange and enables collaboration.
- Compliance. Navigate the regulatory landscape to ensure that data handling practices meet legal standards and industry regulations.
- Lifecycle Management. Oversees data from creation through destruction to make sure it is accurate, consistent, and reliable.
Different individual roles in health data management
There are several professionals and organizations involved in health data management. Looking at the comprehensive stakeholder community, there are efforts to consider and respect their legitimate rights and interests to build and maintain an efficient, trusted, and fair ecosystem. Let’s look at the distinct roles for each group as they relate to data stewardship.
- Researchers. The FAIR guiding principles for research data stewardship (findability, accessibility, interoperability, and reusability) are guideposts for research organizations. These principles provide direction that supports the systematic sharing of data along with related ethical, methodological, and organizational policies.
- Data owners, stewards, and users. These roles are responsible to make sure data is managed effectively and supports the organization’s objectives. Data owners refer to c-suite and leaders who oversee specific data sets and have oversight for its use. Stewards can be subject matter experts (SMEs) who are the go-to for inquiries. Data users are a wider group of staff members or teams who use data for reporting, provide feedback to support continuous improvement.
- Healthcare providers. Clinicians who collect and use patient data for decision making and care improvements. They need to facilitate data sharing and follow data governance policies in doing so.
- Health information technology vendors. Organize and manage data within data governance guidelines for the organization.
- Government agencies. Collect and monitor healthcare data. For example, the CDC’s public health data strategy (PHDS) aims to strengthen the core of public health data, accelerate access to analytics, provide visualization insights to inform action and advance interoperability between health care providers and public health.
- Payers. Use data for reimbursement and benefit design for future programs.
What Is a Data Steward?
Data stewards are responsible for implementing data governance policies, handling data-related requests and maintaining data integrity. Specific responsibilities for data stewards include defining data quality metrics, managing metadata and reference data, tracing data lineage and classifying sensitive data.
Data stewards differ from data analysts who use data analytics to improve healthcare outcomes. Data analysts focus on gathering, sorting, and analyzing data from many sources to support better patient care with improved processes.
Bottom line: Data stewards safeguard the privacy and accessibility of data while a data analyst transforms the data into actionable insights by creating reports and visualizations.
The Data Steward’s Role in Healthcare
Data Stewards have a significant role in managing and safeguarding data. In some organizations there are teams of data stewards, while in smaller or those developing their programs, there may be one person in this position.
The key responsibilities of a data steward include oversight of the organization’s data governance policies on security, privacy, and data quality upkeep. This also includes making sure data access only includes the appropriate staff members.
To do their job well, the data steward needs the right tools. This includes the data warehouse that is the best fit for their organization and the right software to facilitate the operational aspects of data management.
Get Started with Health Data Stewardship
According to the World Economic Forum, the essential ingredient in digital healthcare is not a surprise, it is: data. In this context, the focus for many organizations is on how new digital tools can help physicians and their patients predict, prevent and treat disease with the benefit of personalized care. As the tools evolve, there needs to be a coordinated governance effort to guide the stewardship of the data.
The plan for a true learning health system in the future that advances knowledge based on trustworthy digital technology within the guidelines that meet the ethical and responsible compliance requirements is the ultimate goal. To get there, a robust data governance program and a commitment to stewardship is vital.
Harmony Healthcare IT commits to the stewardship of sensitive personal information and critical business information, in acknowledgement of the many threats to information security and the importance of protecting the privacy of the company’s constituents, safeguarding vital business information, and fulfilling legal obligations.
Harmony Healthcare IT’s information security policies and procedures represent the foundation for its information security program. Information security policies serve as overarching guidelines for the use, management, and implementation of information security throughout the organization.
Looking for a partner who values strong data governance and walks the talk of data stewardship every day?







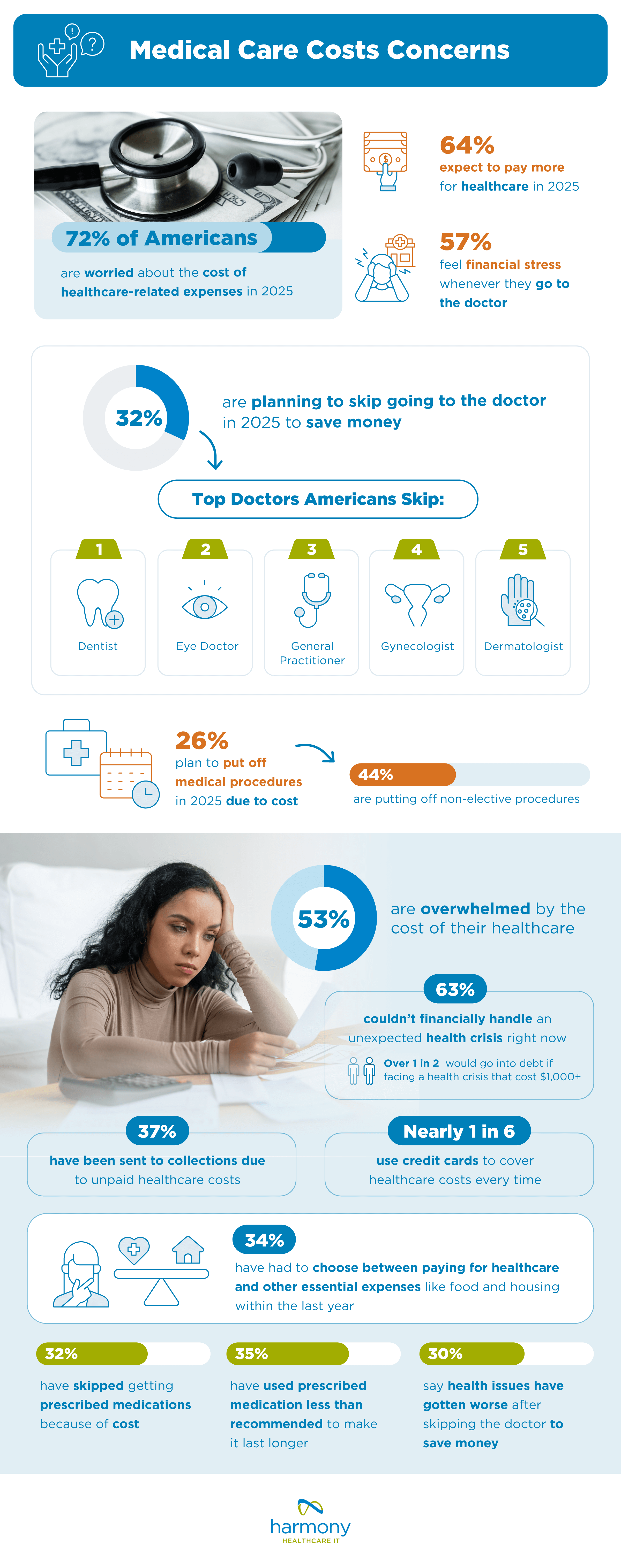 In 2025, nearly 1 in 3 (32%) are planning to skip going to the doctor to save money (
In 2025, nearly 1 in 3 (32%) are planning to skip going to the doctor to save money (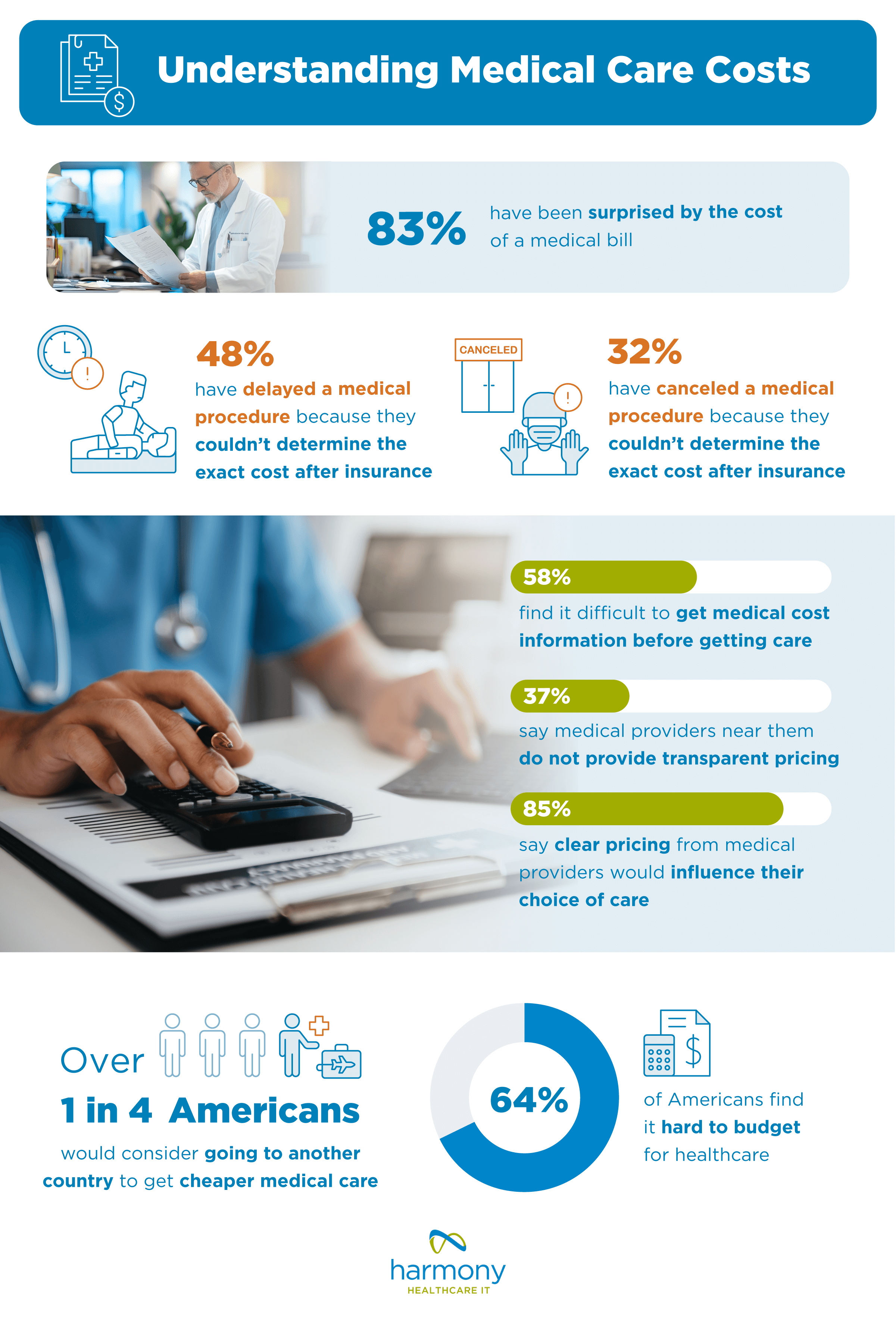 For many Americans, the way medical bills are determined leads to a lot of confusion. Over half (58%) find it difficult to get
For many Americans, the way medical bills are determined leads to a lot of confusion. Over half (58%) find it difficult to get 





