College and Mental Health Report
A day in the life of current college students is very different from how it was five years ago, let alone a decade ago. Our new survey of current college students finds nearly 3 in 4 (73%) find school overwhelming. Mental health plays a big part in the lives of college students, impacting everything from class attendance to grades. For some, it’s even led them to take a leave of absence from school.
How Mental Health Impacts the College Experience
 Over 2 in 3 (68%) college students are stressed about the upcoming school year, and mental health appears to have a considerable impact. Almost half (46%) of current college students have a diagnosed mental health condition, which is an even higher statistic than the previous study we did on the mental health of Gen Z. The top mental health conditions students struggle with are:
Over 2 in 3 (68%) college students are stressed about the upcoming school year, and mental health appears to have a considerable impact. Almost half (46%) of current college students have a diagnosed mental health condition, which is an even higher statistic than the previous study we did on the mental health of Gen Z. The top mental health conditions students struggle with are:
- Anxiety
- Depression
- ADHD
- PTSD
- Insomnia
Mental health is entering classrooms with many students. Due to mental health struggles, over half (51%) of today’s college students have skipped class, 1 in 3 failed a test, and nearly 1 in 3 (29%) failed a class. Mental health struggles have gotten so bad for some that over 1 in 4 (26%) students have been forced to take a leave of absence from school.
44% of current college students say they do not have the mental health support they need at school.
While nearly 1 in 5 (19%) have used their college mental health services, 40% said it did not help. Of those who haven’t used mental health services on campus, 35% said they don’t have enough time, 22% are concerned about confidentiality. In a similar vein, 11% don’t want their parents to know they’re struggling and are worried they’d find out if they try to get mental health help.
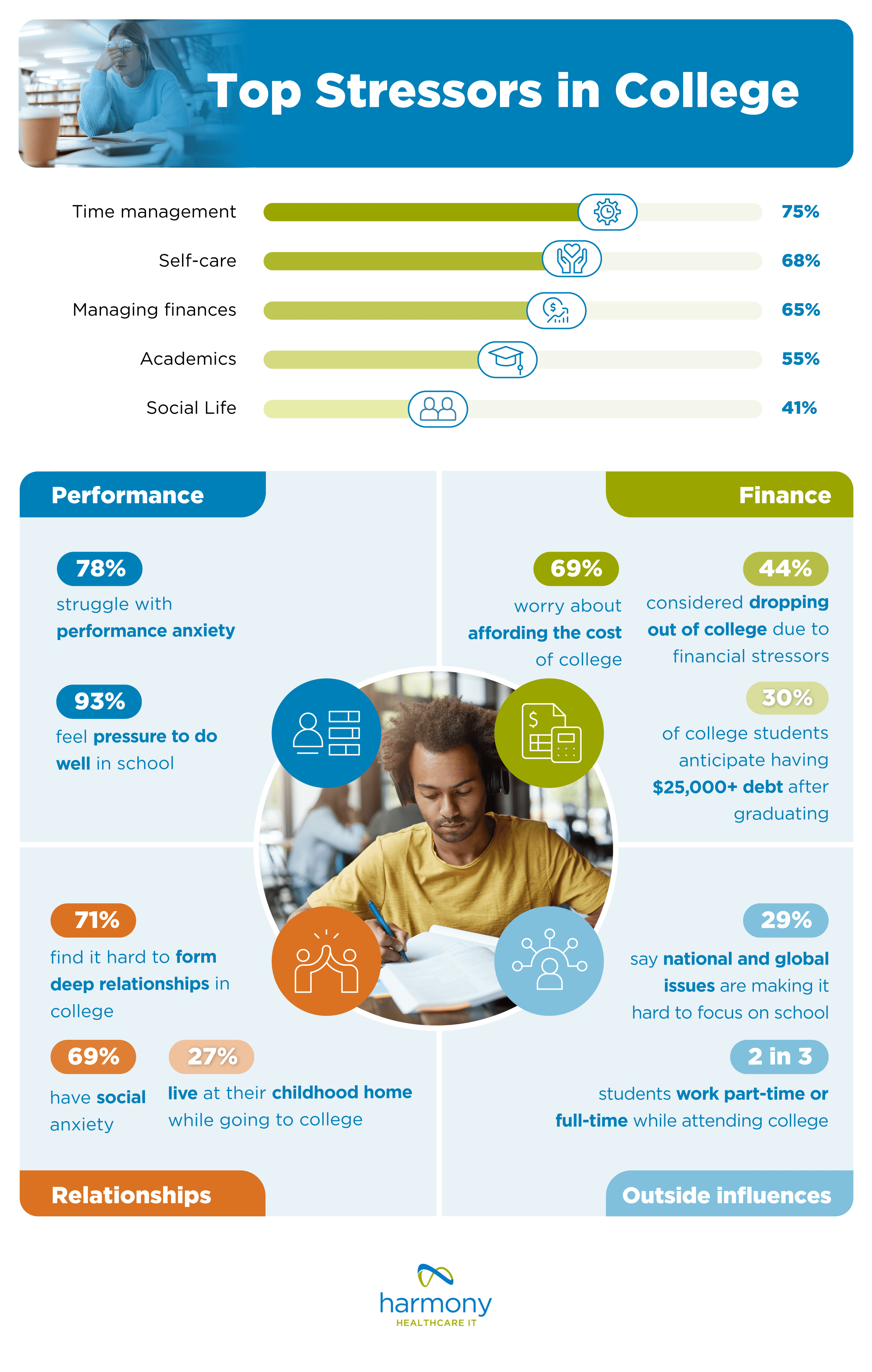
Top 5 Stressors for Current College Students
 Being a college student is not easy. On top of balancing academics, college students are often learning how to live life on their own. The top 5 stressors current college students face are:
Being a college student is not easy. On top of balancing academics, college students are often learning how to live life on their own. The top 5 stressors current college students face are:
- Time management
- Self-care
- Managing finances
- Academics
- Social life
Part of what goes into time management is figuring out the best way to balance studies and social life. 93% of college students feel pressure to do well in school, and while 44% say that’s due to family pressure, 85% find that pressure comes from within themselves. Over 3 in 4 (78%) specifically struggle with performance anxiety, or the need to do well in their classes, sports, activities, etc.
Another form of anxiety many students grapple with is social anxiety, or fear and stress in social situations. 71% say it’s hard to form deep relationships. To make the college experience even harder, some college students aren’t living amongst their classmates. Over 1 in 4 (27%) are attending school while living at their childhood home. Of those, 78% struggle to form deep relationships.
How Finances are Impacting College Students
Financially, 69% of college students are worried about affording the cost of college. This anxiety is so intense that 39% say financial stress has negatively impacted their academic performance, and 44% have gone so far as to consider dropping out of school due to their finances. Over 1 in 3 (34%) have a financial aid scholarship that is contingent on maintaining certain grades or GPA.
According to survey data, 30% anticipate having $25,000 or more in student loan debts after graduating. That may be why 67% of college students work either part- or full-time while attending school.
Impact of Global and National Issues for People in College
While there are timeless issues all students face from generation to generation, each year, students find themselves dealing with unique geopolitical influences that impact their time in school. Nearly 1 in 3 (29%) say national and global issues make it hard to focus on school. The biggest issues that are top of mind for students are the 2024 presidential election (64%), the Israel-Palestinian conflict (63%), and the COVID-19 pandemic (62%).
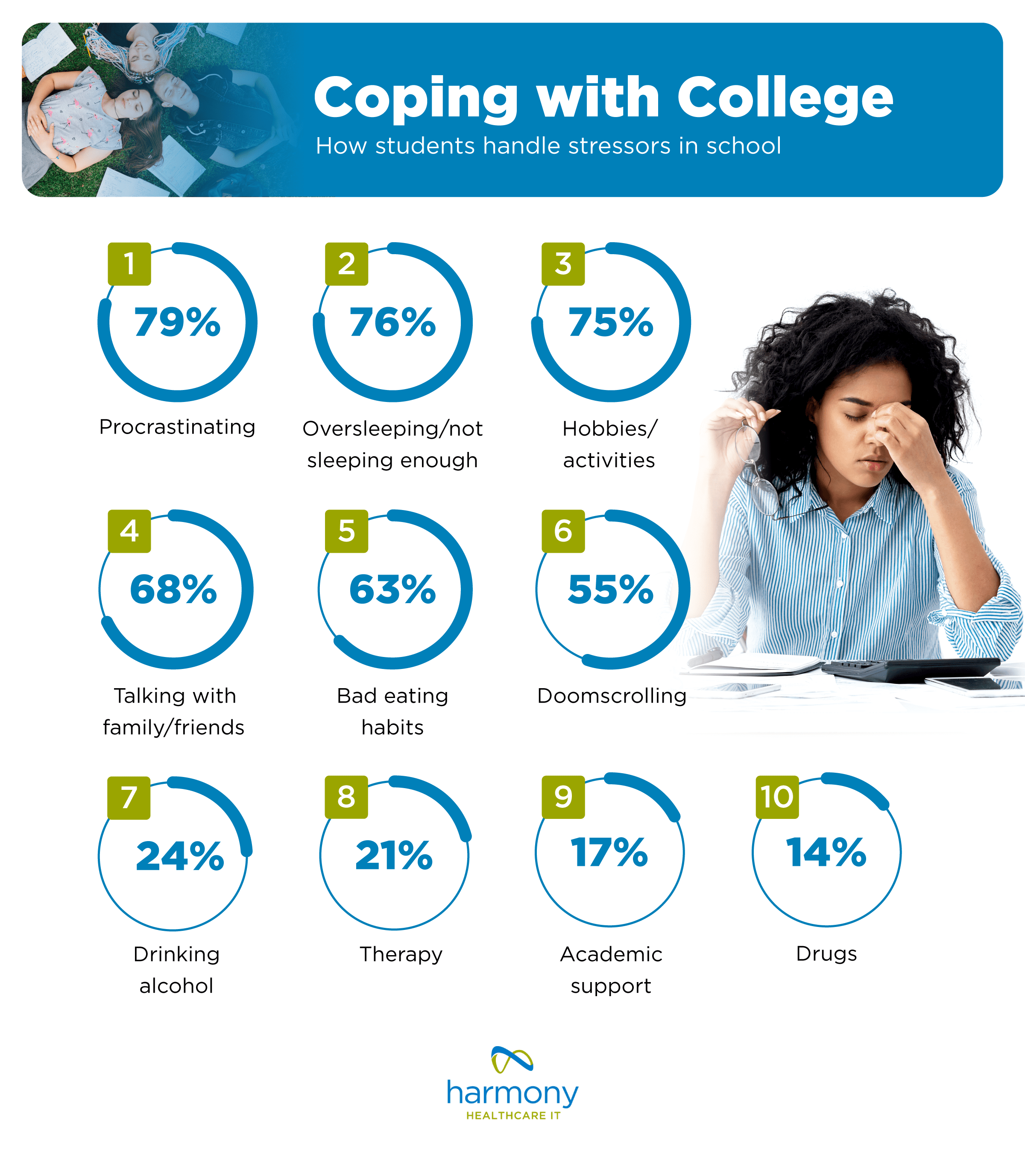
How College Students Cope with School
 There are a range of ways students cope with stressors – some positive and some negative. The top way college students handle stress is by procrastinating. 79% of students admit to procrastination, while 76% share that they oversleep or, conversely, don’t get enough sleep (it’s no surprise since college students are often known for pulling ‘all-nighters’).
There are a range of ways students cope with stressors – some positive and some negative. The top way college students handle stress is by procrastinating. 79% of students admit to procrastination, while 76% share that they oversleep or, conversely, don’t get enough sleep (it’s no surprise since college students are often known for pulling ‘all-nighters’).
Statistics show that 3 in 4 students turn to positive habits such as working on their hobbies or doing extracurricular activities, and 68% talk with family and friends. Others admit to having bad eating habits, doomscrolling on their phones, and drinking alcohol.
College is not an easy transition. It’s a time when students learn to manage all aspects of their lives from academics to activities. While it’s an exciting period of growth, it can be difficult, especially for those struggling with mental health. The college experience doesn’t have to be impossible: focusing on healthy habits, and speaking with a therapist, trusted school advisor, friend, or family member can help so you’re not navigating this new stage of life alone.
Methodology
In June 2024 we surveyed 817 current undergraduate and technical college students. Survey respondents ranged in age from 18 to 63 with an average age of 27. 48% were women, 48% were men, 4% were nonbinary or would rather not say. 10% were first years, 23% were sophomores, 28% were juniors, 31% were seniors, and 8% were in a technical college or program that doesn’t use traditional year designations.
For media inquiries, please contact media@digitalthirdcoast.net.
Fair Use
When using this data and research, please attribute by linking to this study and citing www.harmonyhit.com


 As Senior Director of Data Science at Harmony Healthcare IT, David Navarro drives interoperability initiatives and focuses on the curation and accessibility of data in the healthcare ecosystem.
As Senior Director of Data Science at Harmony Healthcare IT, David Navarro drives interoperability initiatives and focuses on the curation and accessibility of data in the healthcare ecosystem.