For 2020, HIMSS shifted its annual U.S. National Health IT Week to a broader event, Global Health Equity Week. For the first time since its inception in 2006, the week of Oct. 19th now will highlight the role of digital health as a bridge to worldwide patient wellness by focusing on four topics:
- Telehealth
- Public health data modernization
- Patient identification and safety
- Maternal health
Our role as a health data solution innovator continues with even more critical importance as we pioneer and deliver data management solutions that strengthens healthcare delivery, but more importantly, improves lives. As we consider the four pillars for Global Health Equity Week, we recognize the value that immediate access to vital health information offers on a global scale.
Let’s look at how our health data management services support each of the Health Equity topics:
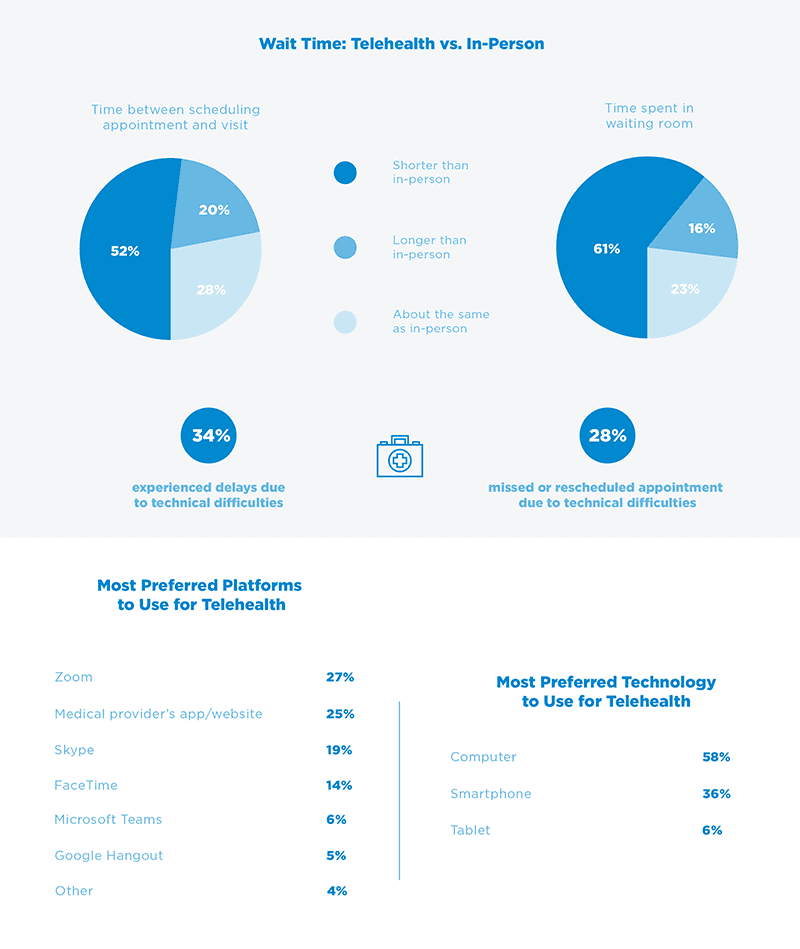
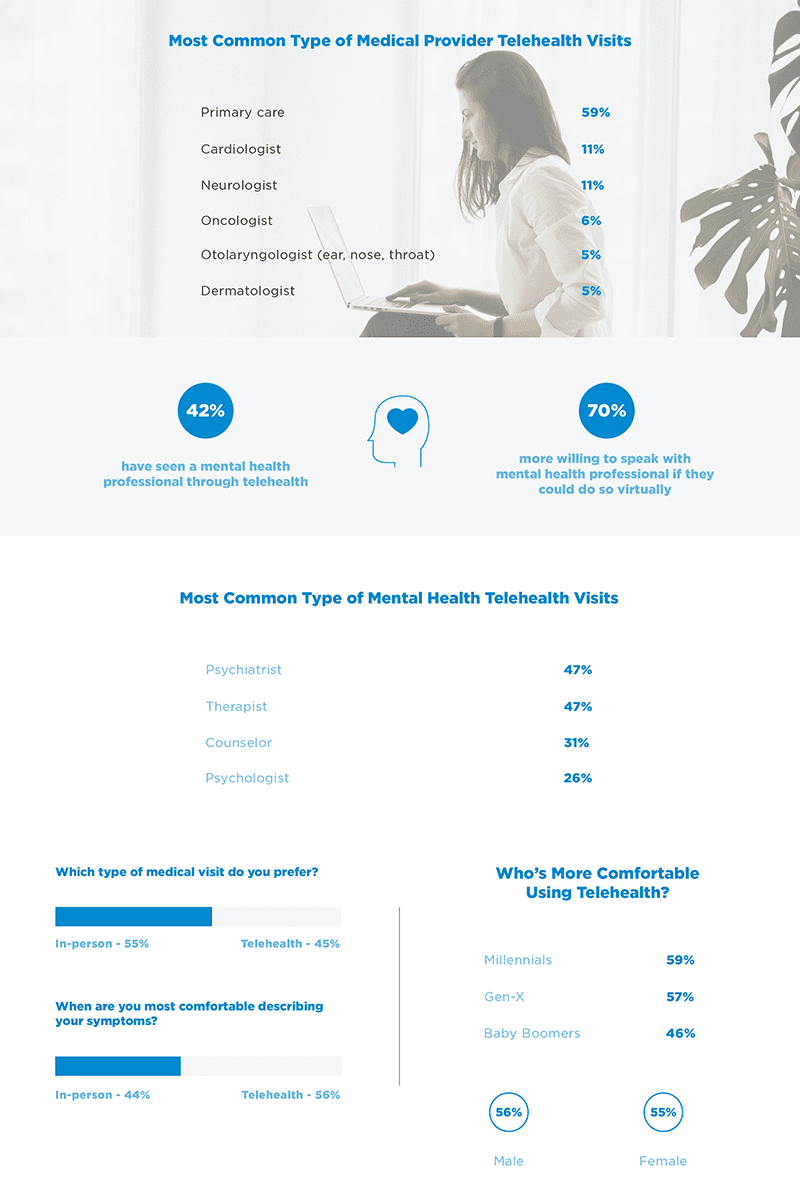
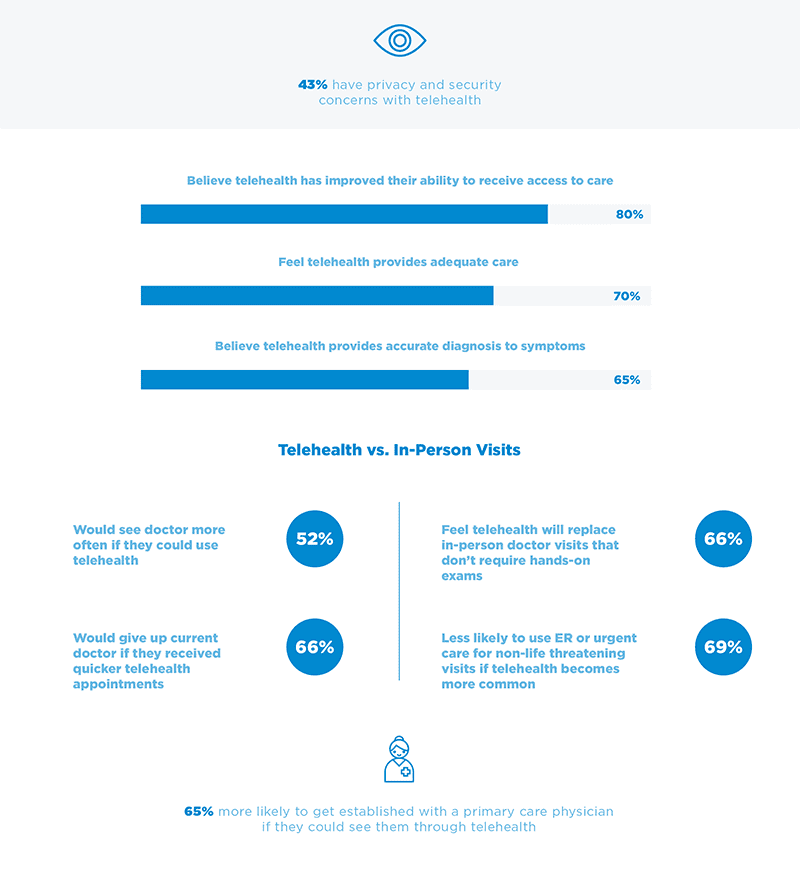
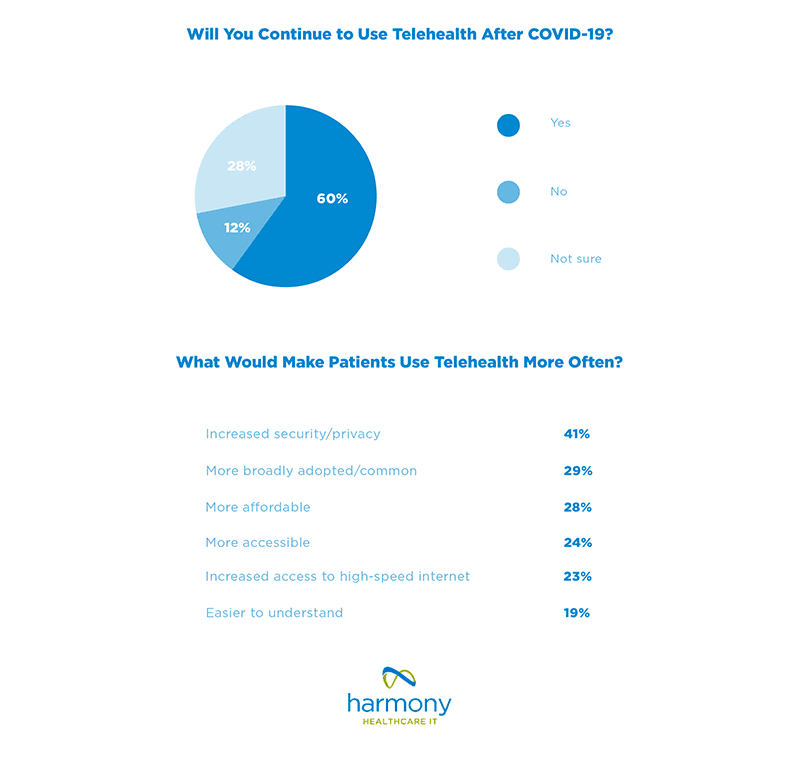
Telehealth – With the recent uptick in telemedicine utilization, access to medical records is important for treatment. Also, the documentation requirements for a telemedicine service are the same as a face-to-face visit. As the trend in telemedicine is expected to continue, there will be EHR upgrades and replacements that require solutions for legacy health data. An active archive like HealthData Archiver® with its Single Sign On capabilities supports efficient and immediate access to legacy health records at the point of care. Further, information flow with telemedicine records is held to the same standard as traditional medical records. This is important to note as compliance to the 21st Century Cures Act Rules on interoperability and patient access to their health records will be enforced beginning in 2021.
Public health data modernization – Data modernization is what we do at Harmony Healthcare IT. Simply defined, data modernization is the movement of data from legacy mainframe databases to modern databases. We help providers of all sizes inventory legacy systems, migrate historical data from siloed systems to a vendor neutral active archive, and then decommission the legacy system. This streamlines the IT portfolio, increases security and provides cost savings. This work also supports interoperability and public health initiatives that involve analytics gained from being able to seamlessly share information.
Patient identification and safety – Experts state that most, if not all, wrong-patient errors are preventable. As migrators of legacy data, we take this part of what we do very seriously, ensuring that patient information is 100% accurate. There has been talk for decades of creating a National Patient ID, which could support patient matching in the future, but until then, there are many processes taking place within different health systems and with EHR and archiving vendors. We remain committed to our integrated data validation process that is a standard feature built into our HealthData Archiver® to give our clients and team real-time communication options within the user interface to easily document and report questions or concerns during validation testing.
Maternal health – The health of women during pregnancy, childbirth and the postnatal period is a key global focus. While it is true that less developed countries have bigger issues, the United States lags behind other developed nations in preventing pregnancy-related deaths. One of the keys to improving these stats is the importance of team-based care, that includes maternal fetal medicine physicians, nurses, obstetricians/gynecologists, cardiologists, midwives and nurse practitioners. Technology-based solutions are needed to provide access to the complete health narrative—such as electronically archived fetal monitoring strips—to help guide treatment decisions and deliver on the quadruple aim in healthcare.
Our team remains committed to delivering technology breakthroughs that lift up healthcare options for all. We fully support Global Health Equity Week and will continue our work in breaking barriers to deliver health information wherever it is needed.
Ranked #1 in the 2020 Best in KLAS Report for Data Archiving, the Harmony Healthcare IT team has worked with hundreds of EMR/ERP software brands, archiving billions of records and storing petabytes of data. We migrate and archive records across the care continuum—for hospitals, health systems, pharmacies, clinics, labs, blood banks, home health care, long-term care, and more.