
With more than 2 million patients admitted each year to over 15,000 skilled nursing facilities (SNFs) in the United States, this market represents about $28 billion in spend annually. The types of care at a SNFs range from short-term post-acute care (including intensive physical, occupational, respiratory, and speech therapy) to intensive nursing care after an injury or illness (e.g., hip fracture, myocardial infarction, stroke). These services are typically for people over the age of 65, and for younger disabled patients.
The merger and acquisition (M&A) activity in the skilled nursing market remains active despite the regulatory uncertainty with likely federal budget cuts of 4.6% or $1.7 billion. There are more than 400 acquisitions expected to close by the end of the year, according to the American Health Care Association (AHCA). This is driven by a new phase of healthcare partnerships for those organizations that can offer consumers access to new services or enhance the delivery of services that require specialized skillsets. For example, some active buyers have their own pharmacy, or their own therapy company and a skilled nursing facility could be a complementary business to add to their portfolio.
A high-performing SNF is an important ally for health systems, particularly those that are focused on performance in value-based care arrangements or looking to enable earlier discharge from inpatient care to the lower-cost skilled nursing setting to help to reduce hospital readmissions.
SNF medical record management is a major consideration during (and after) M&A
Medical records within a skilled nursing facility are highly regulated. There are 175 Federal Regulations that must be followed as well as state rules that may be more or less stringent. For many patients, records are very lengthy as they have lived at a facility for many years. Other patients have shorter stays as the skilled nursing facility is a steppingstone before going back home. Even for a short stay in a SNF, a medical record can be several hundred pages long and include several sections, such as:
- Administrative information – admission fact sheet, hospital transfer forms, any advance directives
- Prior hospital and emergency room records
- Physician orders and progress notes
- Consultations with other medical specialties (podiatry, dental, ophthalmology, optometry, surgical, psychiatry and others)
- Minimum Data Sets (MDS) and Care Area Assessments (CAA)
- Nursing assessments and notes
- Medication and treatment administration
- Skin integrity status (Federal regulation) with strict protocols for weekly and monthly checks for skin concerns and pressure ulcer reporting
- Risk assessments for other neurological testing
- Vital signs
- Therapy (physical, occupational, speech and respiratory)
- Dietary
- Activities and recreational therapy
- Social services
- Laboratory and X-rays
- Nursing assistant documentation
- Other miscellaneous notes
The federally mandated medical record retention requirements for long-term care health information are focused on ensuring the safety, security and accuracy of health records. If state law requires a different retention period, the more stringent between the federal and state must be followed.
Best practices for successful SNF legacy data management during a time of M&A and/or system replacement
As most mergers and acquisitions cause the displacement of one or more systems, it is imperative to have a data management strategy — especially if additional M&A activity is planned. The first three steps include:
- Develop an overall legacy data management strategy to avoid leaving legacy systems up in read-only mode to meet long-term medical record requirements. This is especially important if more M&A is on the horizon, which would also require a solution that securely consolidates protected health information from multiple EMR data sources.
- Evaluate technologies from both healthcare entities to determine which go-forward data systems to use. That includes clinical, revenue cycle, ambulatory, enterprise resource planning (ERP), general ledger (GL), accounting and other ancillary systems. In the SNF M&A transition, one way to reduce cost, labor and risk on the IT side is to decommission data systems that get replaced.
It is important to compile software licenses and service agreements of both entities, including information on the usage scope of licenses, prices for additional or reduced usage and termination provisions. This will assist in making informed decisions about which license agreements to combine, which ones to terminate and which ones to expand. All of these efforts will lead to cost savings.
- Evaluate the organization’s needs for backup, archiving and active archiving as a smart step in managing historical patient and operational data well into the future. It is important to understand the specific differences between data backup, archive, and an active archive:
- Backup creates a copy of data and restores it in case of data loss or corruption.
- Archiving frees up expensive capacity by moving less frequently used data to more cost-effective storage locations.
- Active Archiving is highly scalable storage with intelligent software equipped with workflows for release of information and clinical access. The software uses rich metadata, indexes, directories, tags and more to enable high-performance search and information retrieval.
At Harmony Healthcare IT, we perform EMR data extraction from legacy systems, complete the clinical data migration, and normalize historical data in a relational database and make it accessible in an easy-to-use, browser-based viewer for years to come. If your skilled nursing facility has or will go through a merger or acquisition, visit HealthData Archiver®™ to learn about long-term storage of protected health informaiton as well as HR, GL and accounting data.
Since 2006, our US-based team of experts has worked with more than 550 unique clinical, financial, and administrative software brands used in U.S. and Canadian healthcare delivery organizations. Harmony Healthcare IT has been consistently ranked as the #1 data extraction, migration, and archival healthcare IT company according to Black Book Market Research for four years (2019-2022) as well as ranked #1 in the 2020 Best in KLAS Software & Services Report as a Category Leader in Data Archiving.
Are you facing M&A and sorting through your best options for data management at your skilled nursing facility?


 Nearly 2 in 5 (38%) parents would consider weight loss medication for their child if they became obese. Parents agreed with the recommendation from the American Academy of Pediatrics, noting the youngest age they’d start medication would be 12.
Nearly 2 in 5 (38%) parents would consider weight loss medication for their child if they became obese. Parents agreed with the recommendation from the American Academy of Pediatrics, noting the youngest age they’d start medication would be 12.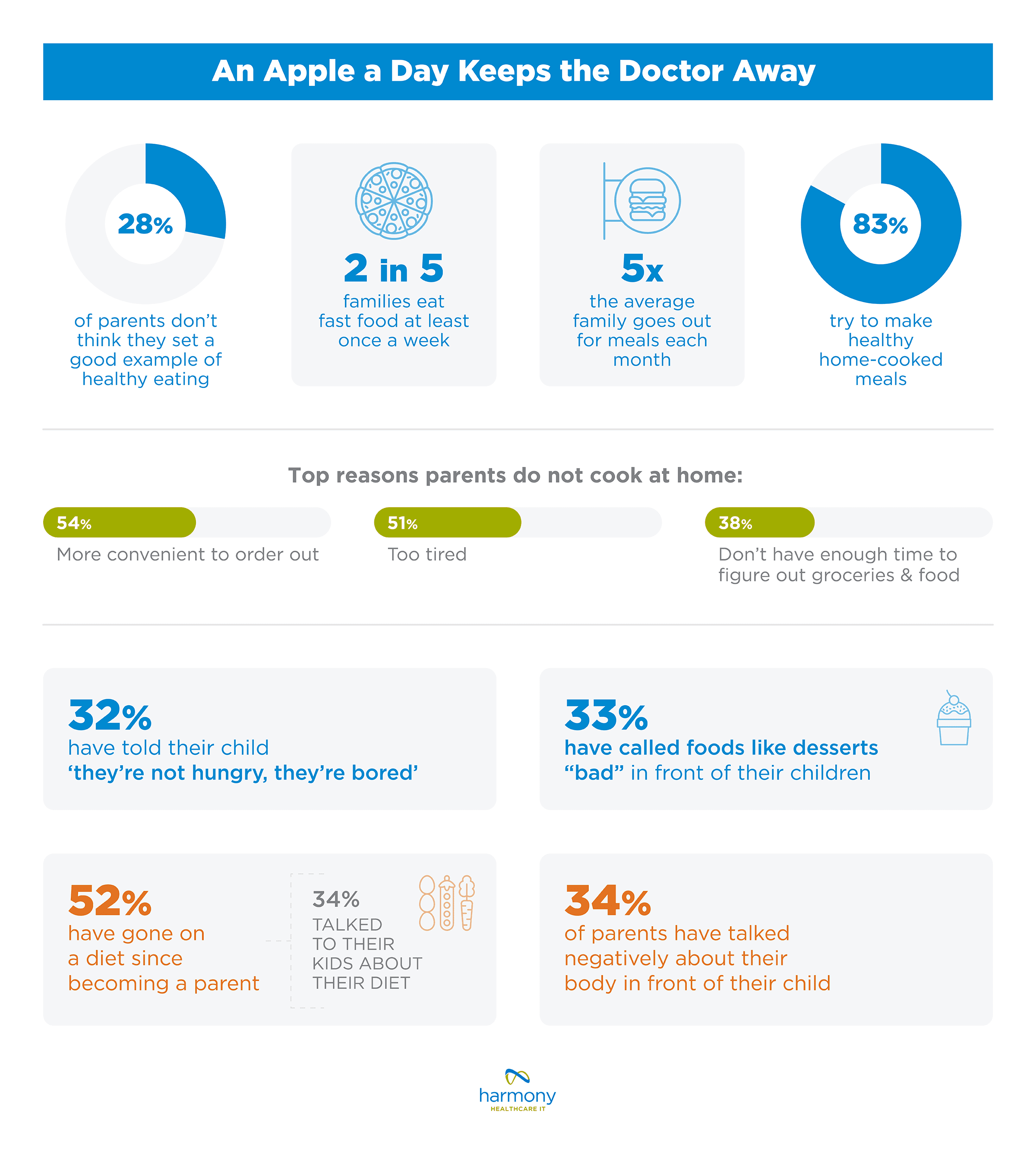 Nearly 1 in 3 (28%) parents don’t feel like they’re setting a good example when it comes to healthy eating. While 83% try to make healthy home-cooked meals, about 2 in 5 (39%) families eat fast food at least once a week. On average, families go out to eat for about 5 meals a month.
Nearly 1 in 3 (28%) parents don’t feel like they’re setting a good example when it comes to healthy eating. While 83% try to make healthy home-cooked meals, about 2 in 5 (39%) families eat fast food at least once a week. On average, families go out to eat for about 5 meals a month. While 1 in 4 exercise with their children, many parents feel like they’re dropping the ball when it comes to staying active. Nearly 2 in 5 (38%) believe they set a bad example about working out.
While 1 in 4 exercise with their children, many parents feel like they’re dropping the ball when it comes to staying active. Nearly 2 in 5 (38%) believe they set a bad example about working out.









