Consider the irony in keeping a legacy financial system up and running with the goal of collecting on outstanding patient billing and insurance payer claims, when the actual costs and risks of maintaining that old system are keeping the meter rapidly adding up more fees.
Collecting from patients and payers can be a timely process
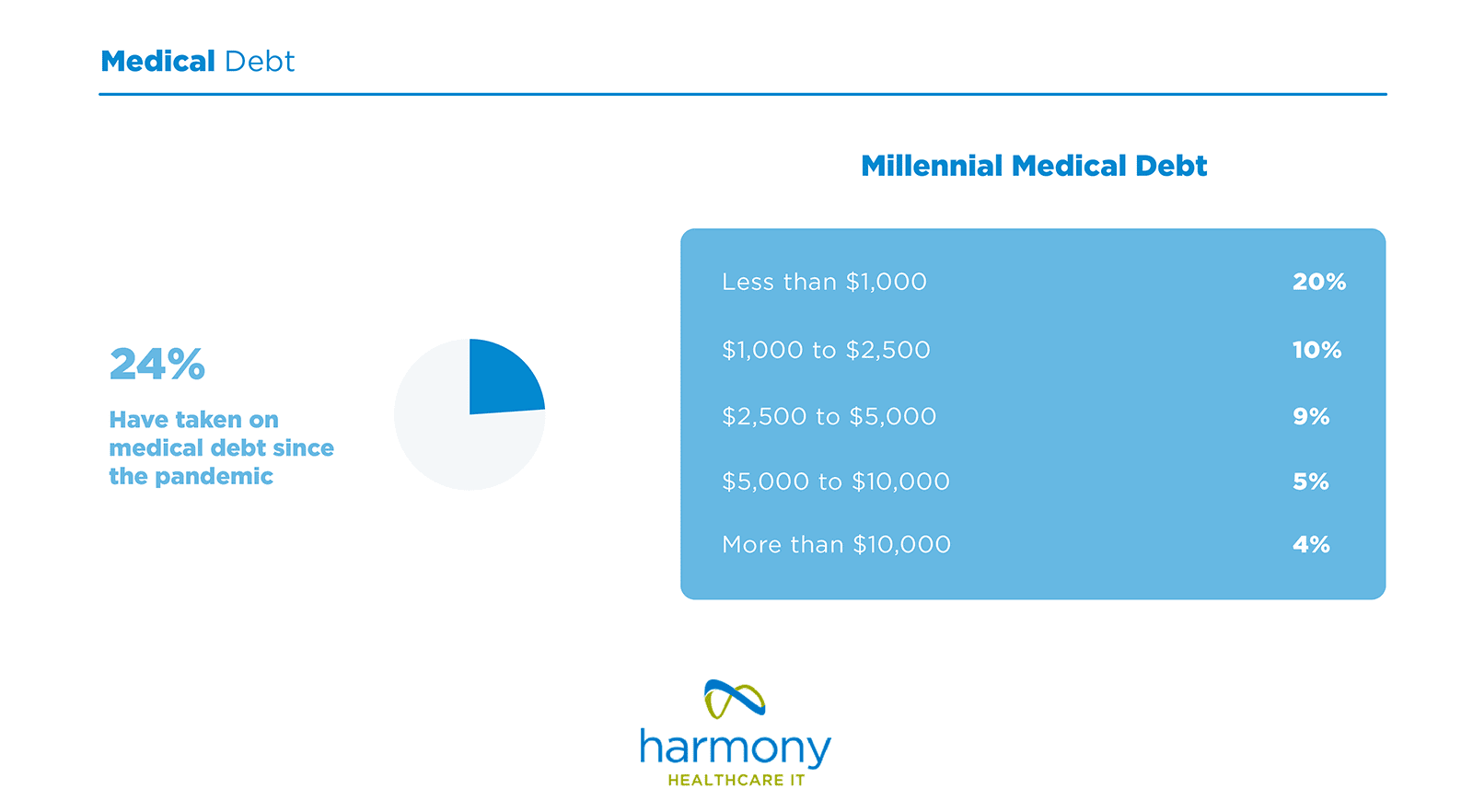
73% of providers report that it takes one month or longer to collect from patients. Further, in 2020, 32% of American workers had medical debt and over half have defaulted on it. Insurers generally pay out claims to providers within 30 days, but there can be delays with coverage denials and numerous other issues with the claim.
Meanwhile, a legacy billing system can keep costs adding up from:
- Hardware and software costs
- Vendor support fees
- Staff training costs to ensure there are employees equipped to work in the legacy system
- Risk of cybersecurity breaches as older systems age and potentially become less secure
Across the IT landscape of numerous industries, 90% of IT professionals say legacy systems are preventing them from taking advantage of the digital technologies they require to be more efficient. However, simply switching billing or other financial systems isn’t a total solution as cash collections in the month following an EHR conversion can dip more than 20%, with one study reporting that by the end of a conversion, the total cash shortfall averaged $168M among US hospitals.
Senior IT decision makers report that modernizing billing systems can boost revenue up to 14 percent annually – over and above the saved operating costs.
However, it’s not as simple as plugging in a new system; an A/R Wind-Down Strategy is Vital
Few billing teams can afford the cost and complexity of completing a financial line-item data conversion to the new billing system. Further, few want to navigate a swivel-chair strategy, working in two concurrent, full-production financial systems at once to wind down A/R – systems with high monthly vendor maintenance fees no less. As an alternative, healthcare providers can decommission the legacy billing system and build their legacy data management strategy around an archiving solution that allows staff to continue collection efforts with complete billing functionality.
This A/R wind down approach:
- Helps maintain continuous account resolution during the system transition
- Reduces costs of legacy system support and maintenance
- Ensures HIPAA-compliant record retention and compliance
- Fortifies defenses against cybersecurity threats to an aging legacy system
Active Archive HealthData AR Manager® supports improved financial performance
HealthData AR Manager®, a comprehensive billing and collections A/R wind down and record storage solution, equips collector to:
- Refile 837 claims
- Receive 835 remittance advice
- View full transaction history
- Post/edit transactions
- Manage collector/agency workflows
- Produce statements/on-demand letters
- Access audit logs
- Monitor predefined interfaces
- Post payments, adjustments, memos, and refund requests
- Produce standard reports and extracts
- Comply with government agency requirements
Important to note, HealthData AR Manager® can optionally integrate with HealthData Archiver® via single sign-on for easy access to legacy clinical records when necessary.
The benefits of an active archive add up to real bottom-line savings
According to a KLAS Research report, 85% of provider organizations maintaining a legacy system that moved to a legacy data archive realized a financial benefit, among other benefits such as consolidating data and improving workflows.
For more detailed information about how A/R wind down with an active archive improves financial performance, visit our website. Or download this AR Management Fact Sheet.
Better yet, reach out and connect with our team.