The electronic dental record, or EDR, is the EHR of dentistry and a contributor to the overall health picture of the patient. Interestingly, adoption of EDR in dental offices in the United States was higher in 2012 than electronic health record adoption rates in medical offices and was not driven by the HITECH program.
Guidelines for the Health Information Technology for Economic and Clinical Health (HITECH) Act authorized $30 billion in incentives to increase the adoption of certified electronic health records (EHRs) for meaningful use, but this didn’t necessarily apply to dental practices that didn’t meet the HITECH requirement of serving a patient population inclusive of a 30% rate of Medicaid beneficiaries.
So as the EDR had a strong organic start, the EHR gained momentum from incentives, leaving the EDR to play catchup.
As of 2017, nearly 9 in 10 office-based physicians had adopted an EHR, and nearly 4 in 5 had adopted a certified EHR. 96% of all non-federal acute care hospitals possessed certified health IT.
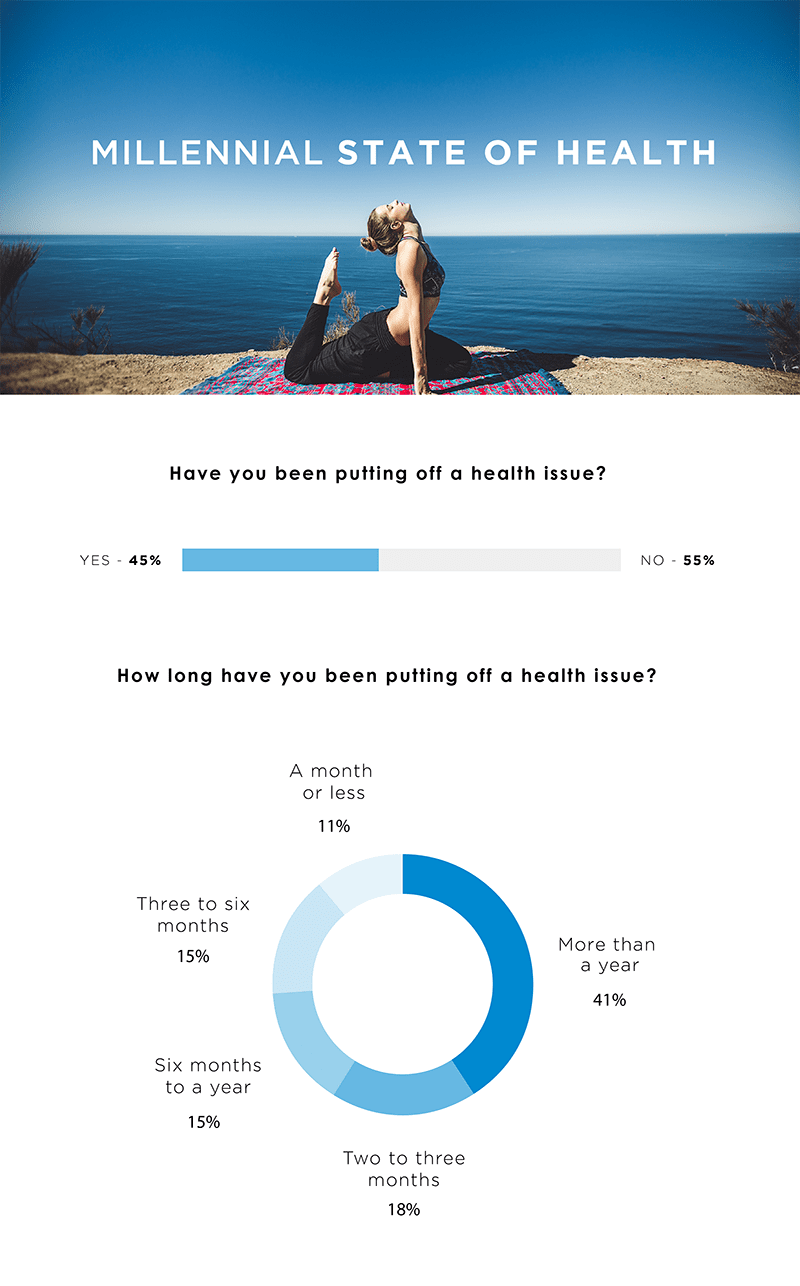
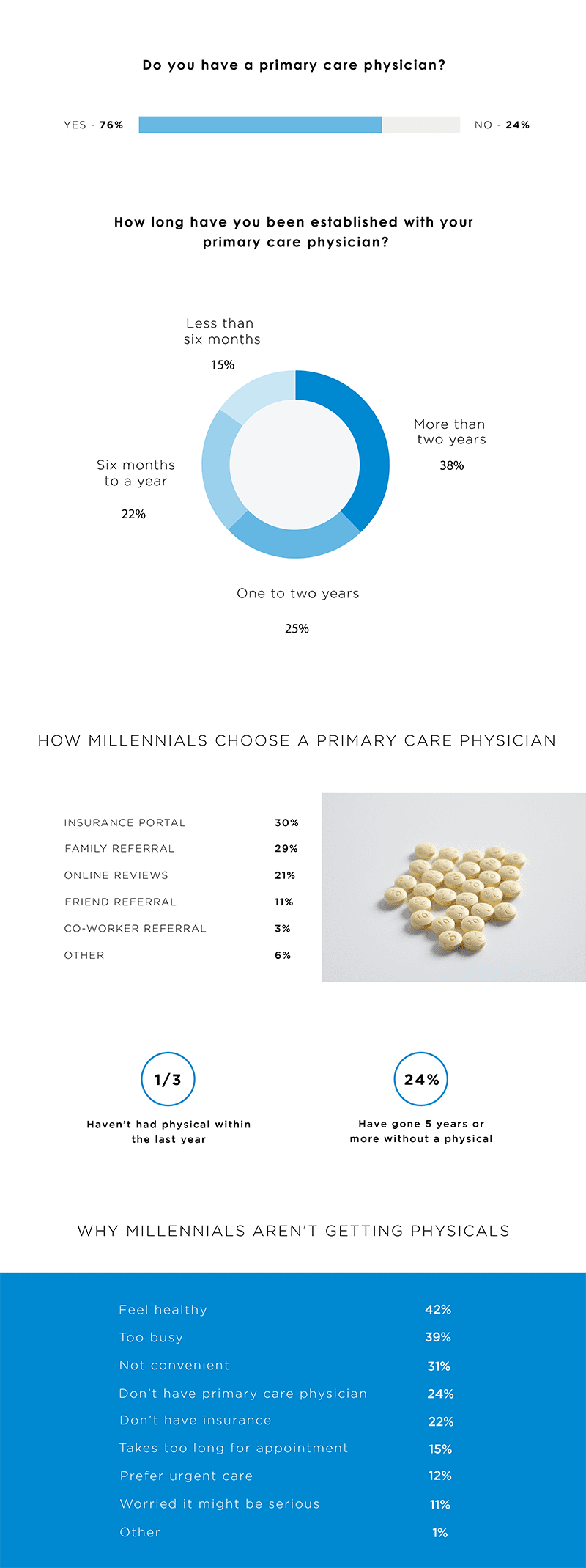
Comparatively, the last several years has seen the overall EDR adoption rate for clinical support to be around 52%. Adoption rates were higher among: (1) younger dentists; (2) dentists ≤ 15 years in practice; (3) females; and (4) group practices, and are once again making swift strides in the marketplace.
All signs point to the dental IT industry being ripe for growth.
In fact, the global Dental Practice Management Software Market is expected to surpass $2.7 billion by 2025, according to a new research report by Global Market Insights, Inc.
This growth, along with the need for efficient record keeping, is driven by two factors:
- Severe periodontal diseases in approximately 25% of people aged 65-74 years old, as reported by the U.S. Surgeon General
- Increased awareness regarding the importance of maintaining oral health, especially among the older population
As the drive for the comprehensive patient health record has become a focus in the medical field, EDR adoption and integration into the dental office continues to increase. Full integration of medical and dental records is an important next step. This linkage already exists in some larger health systems and institutions such as the Marshfield Clinic, and the Veterans Administration system.
Similar to medical records, long term access to dental records is important to patient care and does include retention requirements specific to the industry.
Our team at Harmony Healthcare IT develops and supports HealthData Archiver®, a data management platform providing a single point of access to historical patient, employee or business data for dental and healthcare practices.
The web-based solution, with its release of information workflows, Single Sign-On integrated clinical views, revenue cycle features and eDiscovery capabilities, provides a significant return on investment for dental practices that are switching to a new system and decommissioning legacy systems. The solution consolidates data stores, reduces out-of-production system maintenance costs, mitigates technical risk, and complies with record retention mandates.
An archiving solution such as HealthData Archiver® provides numerous benefits, including:
- Easy, long-term access to dental records that meets retention requirements
- Lower software support costs
- Lower hardware costs
- Decreased cybersecurity risk
Harmony Healthcare IT, an industry leader in data management and archival solutions, recently ranked as the top data extraction and migration health IT company according to Black Book™ Rankings, a division of Black Book™ Market Research.
Looking for guidance on archiving dental records that will keep you smiling? We’re working with dental practices that are making technology work seamlessly for their business.