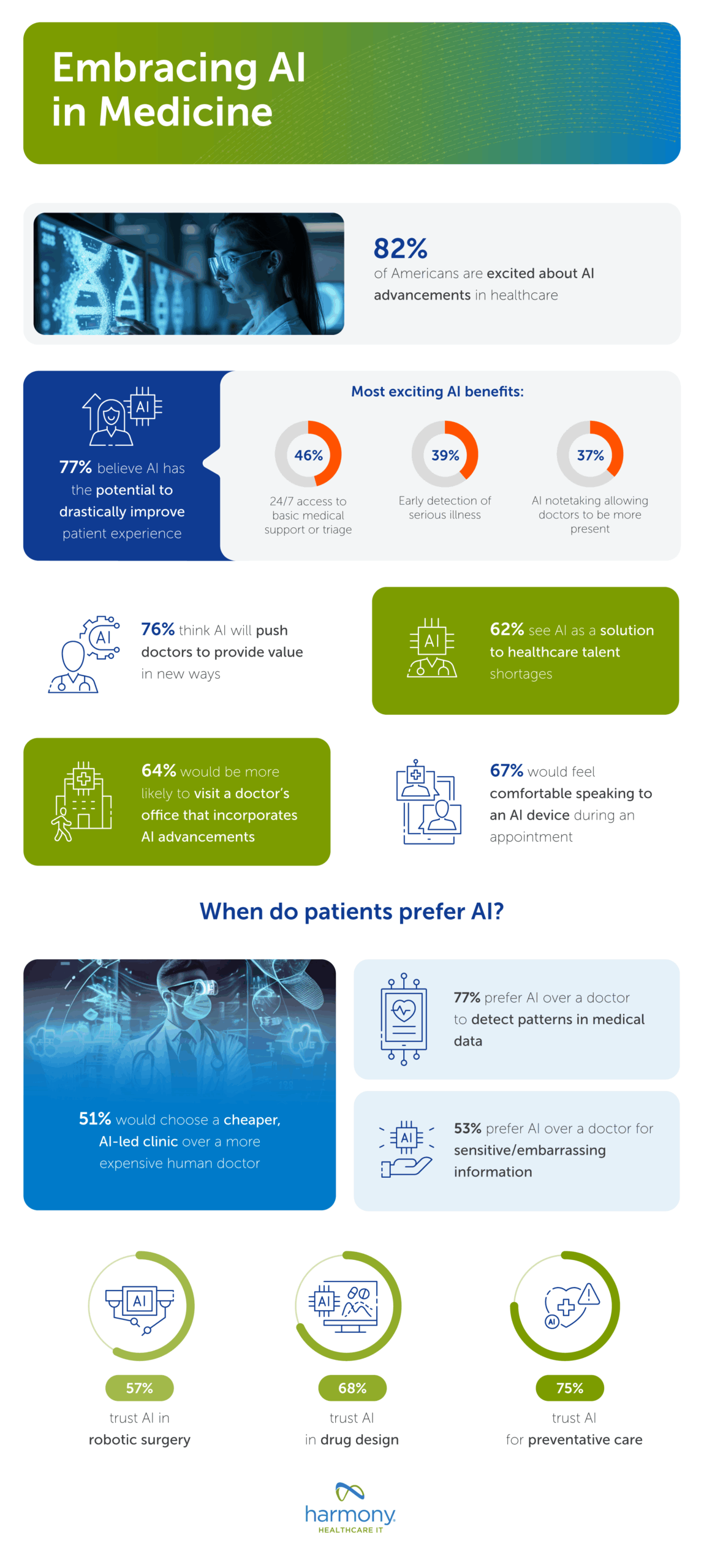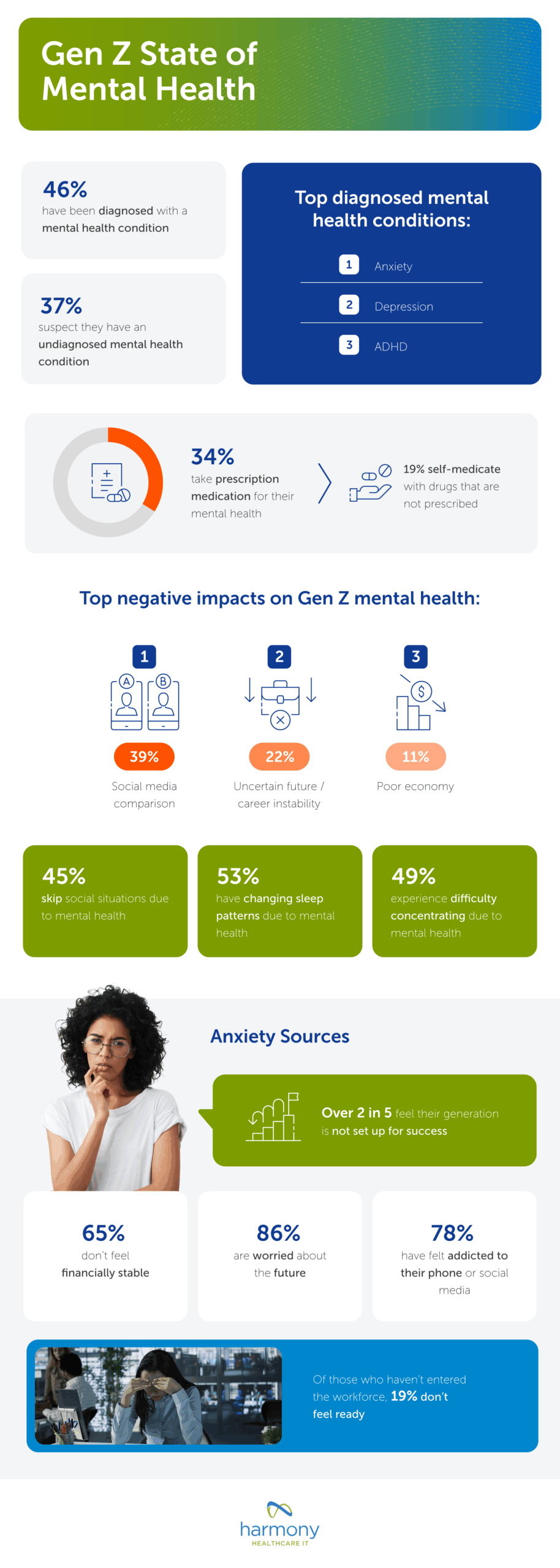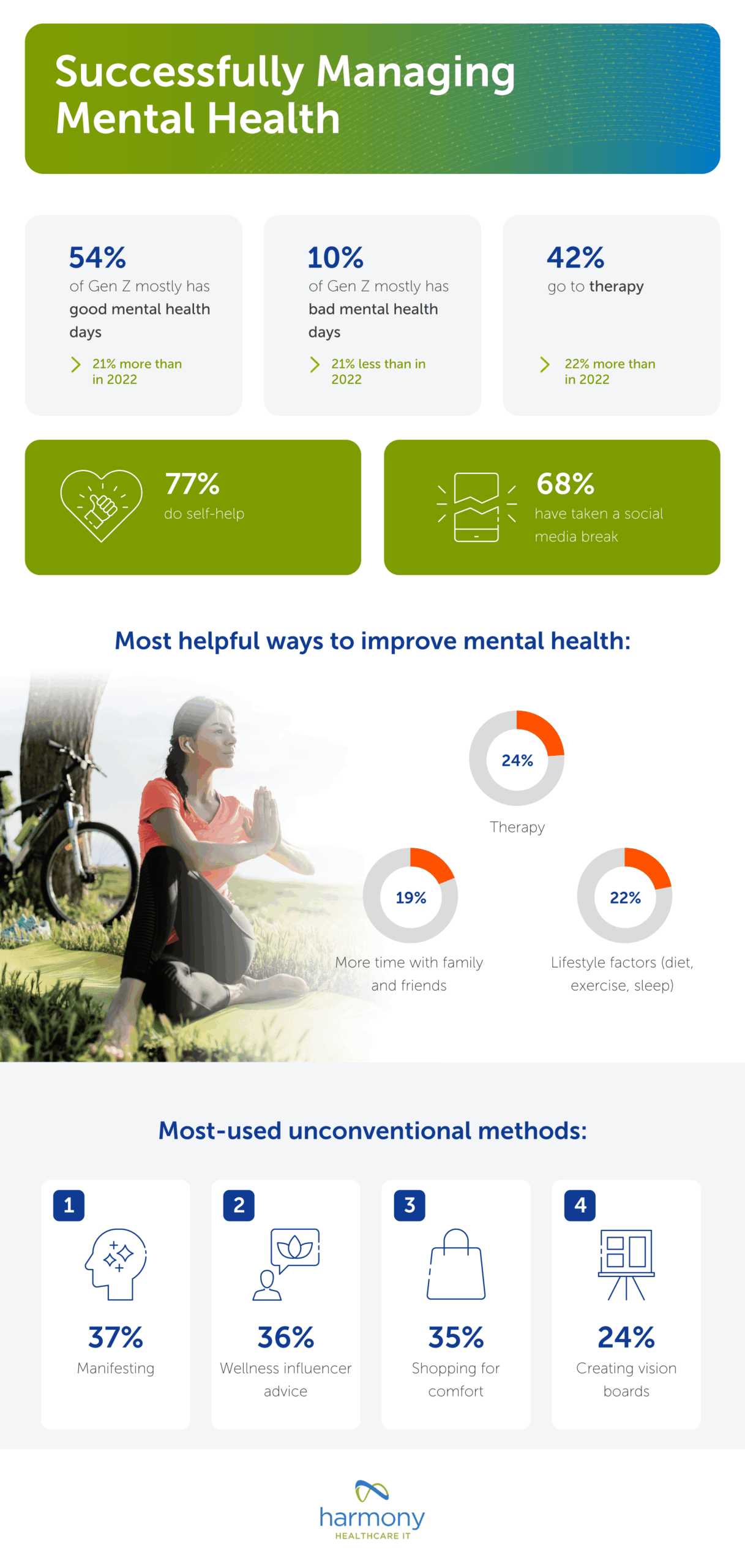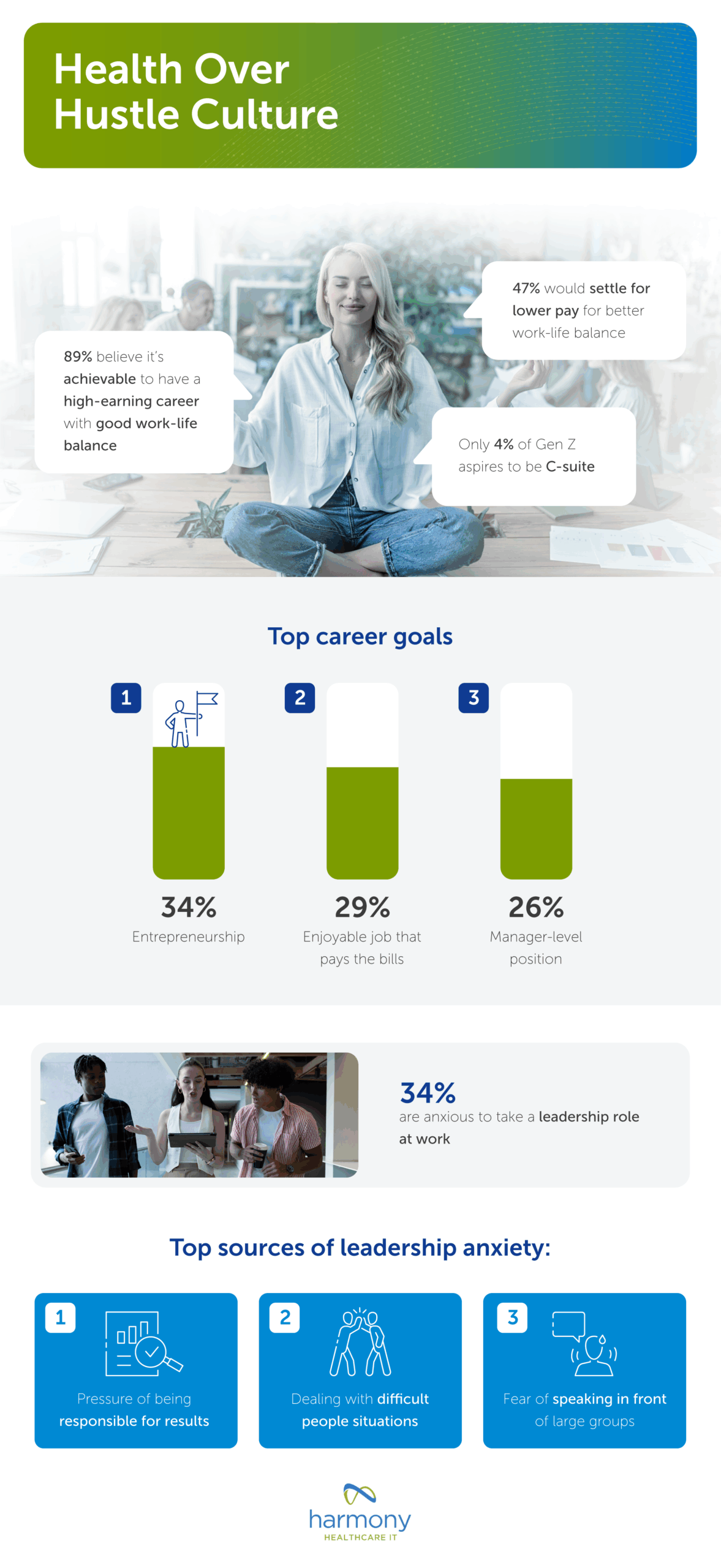
Human capital management (HCM) software has evolved considerably in recent years. Early tools focused on basic human resource management (HRM) functions and administrative support while today’s technology utilizes more sophisticated programs that assist in overall corporate strategy and maximizing employees’ economic value to an organization. Workday and Oracle PeopleSoft are two commonly used HCM solutions. While David Duffield invented both, they are two separate companies, each battling for their piece of the healthcare HR management solutions market.
PeopleSoft, founded in 1987, was the first client-server HR system. It was acquired by Oracle in 2005 to become part of the world’s second largest application software company. Duffield went on to start Workday Human Capital Management (HCM) that same year with its cloud-based (through IBM) HR management solutions that include compensation, payroll, shift scheduling, time tracking and more.
Workday and PeopleSoft market share and deployment options
PeopleSoft and Workday control 37% of the HRM market. Currently, Workday has 22.3% market share, while Oracle PeopleSoft has 14.5%.
Choosing which application to utilize, or switch to, is often based on cost and functionality. One of the key differences between these two applications is their deployment options.
- Workday is on the cloud, which may mean a lower total cost of ownership over other applications since on-prem hardware nor infrastructure is required.
- PeopleSoft can be deployed to the cloud or on-premises. It is marketed for its intuitive user experience, customizable configurations, and ability to deliver actionable insights.
To determine which tool is the best fit, healthcare organizations must assess many factors including their own availability of IT and specialized support staff who may be needed to create and maintain a customized solution.
Replacing HR software tips-off a need for legacy data management.
After determining which solution works best with your ERP or HR strategy, it is time to determine how much data to convert into the new system when replacing PeopleSoft or Workday, and what to do with the legacy records.
That’s where data archiving comes in. Think of data archiving like the side car to your go-forward application after replacing an HR system, providing access to legacy HR/HCM data with secure, Single Sign-On from the active new system.
Cost savings and ongoing access to employee and business records are leading benefits of archiving.
An archive supports compliance with record retention requirements from the IRS, Fair Labor Standards Act (FLSA) and the U.S. Equal Employment Opportunity Commission (EEOC) and other state level organizations. There are HCM requirements to retain records such as:
- Payroll (time and attendance)
- Personnel files
- Medical records
- FMLA documentation
- Tax records
- Hiring records
- Performance appraisals
- Overtime hours
- Job applications
- I-9s
An archive helps ensure ongoing access to records and provides cost savings from removing legacy vendor licensing fees and maintenance contracts. There are also soft costs to consider such as the time and effort it takes to maintain multiple applications in the portfolio.
Ready to have a conversation about your HCM data migration project?
Our team is equipped and ready.
We specialize in legacy record storage and release and have migrated and archived data from PeopleSoft, Workday and more than 700 other software brands for providers nationwide. Harmony Healthcare IT consistently ranks as a standout for archiving the largest and most complex clinical and financial software systems. We also received all A’s in the six customer experience pillars of culture, loyalty, operations, product, relationship, and value. These achievements underscore our steadfast commitment to keeping patient, employee, and business records accessible, usable, interoperable, secure and compliant for decades to come.
Let’s connect.
This blog has been updated from the previous version published June 21, 2023.